7 Unexpected Ways to Make Healthcare An Anti-Anxiety Experience Through Design
Few would challenge the fact that healthcare systems around the world were amongst the most significantly impacted industries of the COVID-19 pandemic. Healthcare providers were forced to ask much more of their systems resources while dealing with a materials distribution system ill-equipped to provide for the sudden needs of a pandemic and therefore straining its ability to assure doctors and nurses of their safety in a time of extreme need.
In the wake of the aftermath, as the dust slowly begins to settle and the pendulum begins to find equilibrium, anxieties run deep and emotions are high around healthcare, prioritizing its importance both on an individual, and collective, basis more than ever.
With the center of the healthcare experience shifting away from the traditional understanding of the hospital or doctor’s office, and towards instead the patient themselves, it’s important to evaluate human-centric design now more than ever.

OhioHealth Free Standing Emergency Department
Consumers are looking to be recognized as humans and valued as individuals, taking active control of their health now more than ever. A 2018 Deloitte healthcare industry study predicted that by 2040, spending on preventative care will outpace that of disease management. A lofty goal, but one that most healthcare experts agree can both reduce the cost of healthcare and provide a higher level of care for those in need.
As we reflect on, and respond to, rising concerns centering around mental health, it’s important that we consider the built environment’s ability to influence and support mental well-being for all of those users that occupy healthcare-driven spaces. We must recognize our responsibility as designers to create space for change that supports everyone on the journey, from patient to provider, and inspired by my years of experience collaborating with visionaries in the industry, and an award-winning team at MA Design. We’ve developed 7 unexpected ways to make healthcare an anti-anxiety experience through design.
1. Providing the Path through Wayfinding
A patient visit doesn’t begin at the moment a patient arrives at a healthcare office or campus…it actually begins when that visit is scheduled, and the first step in relieving patient anxiety is with a clear and consistent set of instructions about their visit – such as when and where to arrive, what to bring, and what to expect throughout their visit. Once the patient has actually arrived at their destination, messaging, visual cues, and landmark elements consistent with the prior instruction help to provide directional understanding and flow, and are imperative to eliminating anxiety. This consistency and comprehensive information allows the patient to immediately feel like they have an understanding of where they are, where they’re going, and how they’ll get “there”, allowing them to feel more in control and comfortable with their surroundings, which is particularly critical in times of emotional stress and potentially physical challenges. It’s also important that the verbiage used for healthcare wayfinding systems is in sync with the lexicon used by its staff and providers, to create consistency and eliminate confusion, instantly decreasing anxiety. For example, if someone refers to a certain area of the hospital as the “West Wing” but all directional signs label it the “Yellow Tower”, it instantly creates a disruption for the patient. Instead, make training staff and providers a priority to create a consistent brand language. While signage is a critical component of this process, fewer words and more visual and graphic elements can help to reduce anxiety and quickly communicate directional cues.

Pediatric and Low Vision Rehabilitation Clinic – The Ohio State University
2. Minimizing Over Stimulation + Triggers
Patient experiences during the COVID-19 pandemic have generated discussions about the place of waiting spaces in healthcare environments. Waiting was simply not possible for a period of time in some instances, so healthcare providers were forced to make abrupt changes to where and how people were queued up to receive their care. While the elimination of waiting spaces in healthcare settings may be a welcome change to some, as waiting spaces are costly, do not generate revenue, and consume a significant amount of space in designs, accommodations must be made for patients before they are seen. Technology may provide some solutions by enabling us to alert hospital clinical staff upon arrival, and digital apps can provide for queueing and even helping manage expectations and wait times.

Memorial Health Belpre Cancer Center
The traditional “Waiting Room” experience is one that should be seriously evaluated in the next evolution of healthcare – directly supporting better mental wellness. How? Sitting in a waiting room for a test or procedure, and seeing another patient near you in an emotional distressed or visibly injured condition can be incredibly triggering, especially while waiting on edge for your name to be called, or feeling pressed for time, while the surrounding world buzzes loudly around you. Any of these conditions individually, let alone when combined into one setting, can create an incredibly over-stimulating environment and significantly increase stress levels. Instead, allowing patients the opportunity to control their experience, walking in only when it is their time to be seen, and reducing elements like noise, an example of a trigger, that accompanies the in-building waiting experience, can all be a part of reducing this over-stimulation.
3. Destabilizing Healthcare Design
Chances are you’ve been there – as the patient, sitting in the exam room waiting for your doctor, on a cold and institutional table covered with noisy and uncomfortable wax-coated paper, surrounded by dispensers of latex gloves, sterilized medical equipment, and medical disposal containers. Maybe you’re attempting to distract yourself mindlessly by scrolling through your phone, or perhaps staring at the gray wall in front of you wondering when you’ll be seen and if that’s the doctor’s voice you hear next door. Nothing feels more isolating and uncomfortable than this experience. It is quite the antithesis of what progressive healthcare providers are striving to accomplish, but far more common than it should be. Enter biophilic design – increasing occupant connectivity to the natural environment in any way possible – as a means of reducing anxiety. Through the incorporation of natural elements and materials, we can create environments that are much more conducive to providing an appropriate setting for patients. Providing outdoor spaces at ground level or on rooftop green spaces, or even in indoor gardens if the climate or location are challenging, can provide the kind of respite needed. Windows providing access to light and views, and if access to natural light isn’t an option, allowing patients to determine their view on digital screens or with augmented reality devices can be a surrogate. Attentiveness to other environmental stimuli, such as sounds and smells, is just as important in completing the environment in biophilic design, however careful attention to the specific needs of the occupants of a space can dictate what is appropriate, and does not create its own over-stimulation or negative reaction.

Heart and Vascular Specialty Center
Lighting is an under-considered element of design with an overwhelming impact. Lighting levels and the control of them can have a huge impact on the space, and usually are much less expensive than other options. Take, for example, the idea of entering a respite room – with dappled, dim lighting and deep, rich wall colors that make you feel comforted and at ease, versus walking into a fluorescent environment with sterile, alarmingly bright, white walls. Two environments are utilizing all of the same elements, but with the control and strategy of lighting at its core, the experience is entirely different, and far less anxiety-inducing.
4. Designing the Patient Support Zone
For many, the chance to have family or friends near them during times of critical healthcare was taken away amid COVID concern and was a major source of frustration for many who were receiving care. Once the pandemic is behind us, this privilege will be prioritized more than ever and consideration should be given to how the patient’s personal support team can be better accommodated in the event of future pandemics.

OhioHealth Riverside Methodist Hospital
We rely heavily on the support of loved ones when faced with receiving health care, whether at home, in a patient bed, or simply getting assistance or mental support during a routine visit. The built environment in a healthcare environment must reflect this, and provide for processes and spaces for comfort in the “patient support zone”, where these special people can feel they have a place to belong during the provision of care for their loved ones.
5. Making Safety + Security Humane
The traditional concept of safety – from a security perspective – has been trending as an increasing concern among healthcare facilities, with hospitals even needing to install security measures such as metal detectors in emergency departments as an example. The priority of safety is a consumer sentiment that will spread into all industries, demonstrated by the skyrocketing of home security system sales in 2020. The concept of safety and security now also includes sanitization, as disease control is something people are hyper-aware of. Respecting and adhering to COVID protocol is a high priority regarding patient and caregiver safety, and safety is huge for managing feelings of stress and anxiety. According to Google Trends, sterilization is a 2020 breakout global search term (it grew by more than 5,000%).
Combining perspectives on the variety of issues that make up safety in security in a healthcare environment will be a constant challenge. The process of screening those entering a healthcare facility, whether to prevent physical harm or biological harm, will be a key consideration in healthcare design, however, the most successful designs will also maintain a welcoming environment combined with personal privacy and dignity for staff and visitors.
6. Disguising Disruptions
Medical devices and equipment are certainly visual triggers for many, if not most, triggering the brain to recognize the severity of the situation and stimulating the release of cortisol and adrenaline as a stress response. Instead of having these on display, strategic design thinking provides for these devices to be disguised, which with proper planning consideration by healthcare design professionals working closely with healthcare providers is an accomplishable feat, and directly reduces anxiety for the occupants.
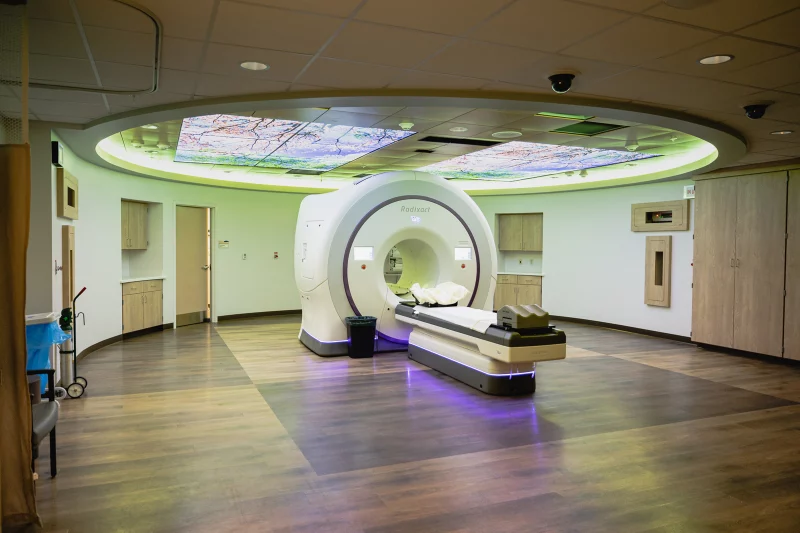
Memorial Health Belpre Cancer Center
The goal for the design of healthcare spaces is not necessarily to hide everything from the sight of the patient, and in doing so, give the patient the perception of being less in control and less understanding of the care that is being delivered to them. Instead, giving patients adequate insight and understanding of where they are and what is happening around them will help to ease their mind as they are educated and brought along by those who are caring for them.
Certainly, there are spaces within a healthcare environment where the role of the designer is to create a comfortable experience. In the case of some radiation therapy delivery models, a patient may be surrounded by equipment that extends well beyond the limits of the room they perceive, sometimes even a floor above and below, and surrounded by thick concrete and steel walls. These spaces can be appropriately designed and effectively not alarm a patient with the complexity and enormity of the equipment and processes delivering healing care to them. How we design creates a human experience, and the focus must be on a calming experience with the surroundings, colors, ability for the patient to have comfort, choice, and control – and of course, disguised disruptions.
7. Separation for Support
Creating separate areas for patients and providers allows for a separation of roles, providing for safe and efficient circulation for patients and visitors while providing spaces for providers to decompress “off stage” and recharge. This can be accomplished in a number of ways depending upon the culture and preferences of a healthcare system. One example, the central core model of design optimizes this concept, where the healthcare providers are located central to the planning model and can be applied to clinical areas, diagnostic and treatment areas, or patient room areas. While less traditional, this more modern approach to design creates staffing efficiencies, enables effective staff interaction and support, while largely separating patients from clinical traffic. It also carries a number of benefits regarding the distribution of medical supplies that need to be stocked in the patient care spaces. As an advocate for this model, I feel that it is one that should be discussed amongst the planning models when designing new healthcare spaces, and realize that it may be a fairly drastic departure from traditional planning models and therefore deserves appropriate investigation and testing before a new model is implemented.

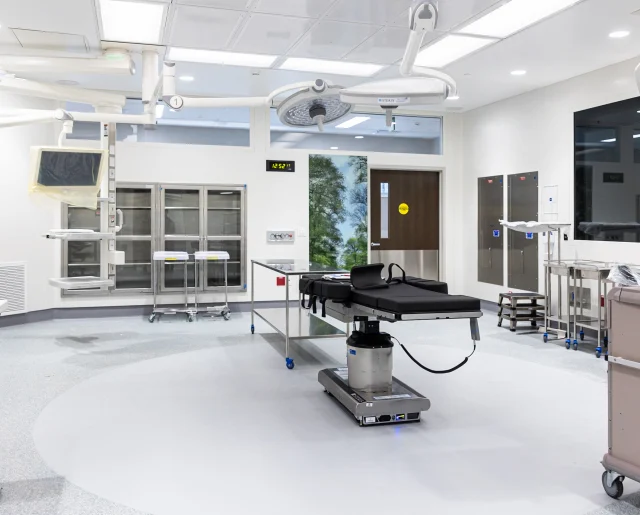
Mount Carmel Grove City Outpatient Surgery Center
Conclusion
The entire sequence of the healthcare experience offers opportunities to support the mental health of patients and visitors, as well as the providers, making healthcare facilities and campuses an anti-anxiety experience by design. The details in these touchpoints drive the human experience, demonstrating the value of the patient in this consumer-driven approach through well-activated design.
If you’d like to continue the conversation or learn more about the ways our architects and designers can partner with you to create space for change, please feel free to contact me at jonathanw@designwithma.com